icon
Moisture-associated skin damage
Moisture-associated skin damage (MASD) is an injury to the skin by repeated or sustained exposure to moisture. There are four common types of MASD:
- Intertriginous dermatitis
- Incontinence-associated skin dermatitis
- Periwound moisture-associated dermatitis
- Peristomal moisture-associated dermatitis
For any of these four types of skin damage, long-term exposure to moisture can lead not only to redness and inflammation, but also to skin erosion and/or infection.
Intertriginous dermatitis (ITD)
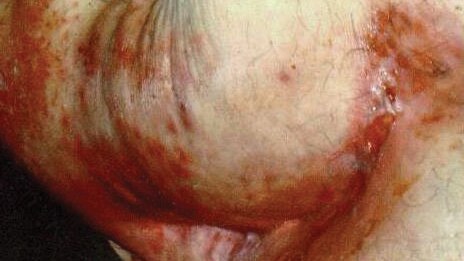
Non-caustic moisture damage: perspiration
Inflammation in skin-to-skin or skin-to-device related to perspiration, friction and bacterial/fungal bioburden. Characteristics include erythema, itching, maceration, erosion and odor (possible satellite lesions).
Interventions
- Assess and treat the cause.
- Gently cleanse the skin fold daily with a pH-balanced, no-rinse skin cleanser. (Bedside® Care Foam Bedside-Care EasiCleanse™ Bath)
- Pat dry or air dry.
- Place InterDry® Ag in the skin fold or under the medical device.
- Allow 2 inches to be exposed to the air.
- Date and initial InterDry Ag.
- Reposition as needed.
- Replace if soiled with urine, stool or blood.
- Discard after 5 days of use.
Incontinence-associated dermatitis (IAD)
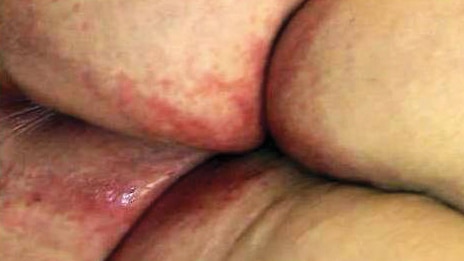
Caustic moisture damage: stool/urine
(More commonly known as diaper rash). Inflammation of the skin that occurs when urine or stool comes into contact with perineal/perigenital area, inner thighs, buttocks, or adjacent skin folds. Characteristics include inflammation and erythema with or without erosion or denudation.
Interventions
- Assess and treat cause of incontinence.
- Use a urinary and/or fecal containment device. Consider using a Male External Catheter (Conveen® Optima) for men.
- Offer toileting at least every 2 hours, as appropriate.
- Cleanse skin at time of soiling with a gentle no-rinse cleanser (Bedside-Care® Foam).
- Apply a protective moisture barrier ointment (Critic-Aid® Clear or Baza Cleanse & Protect® Lotion) to the affected area.
- Apply a topical antifungal treatment (Critic-Aid Clear AF or Baza® Antifungal), if needed.
- Consider using underpads or absorbent briefs.
Periwound moisture-associated dermatitis
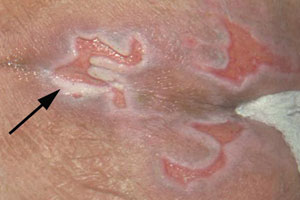
Caustic moisture damage: wound exudates
When wound exudate has sustained contact with the skin, skin damage is the likely outcome. Characteristics include inflammation and erythema with or without erosion.
Interventions
- Assess cause of periwound damage. If wound is exuding large amounts of exudate, consider using an absorbent dressing (SeaSorb® Alginate or Biatain® Foam Dressing).
- Cleanse the wound at time of each dressing change with a saline-based wound cleanser (Sea-Clens® Wound Cleanser). Pat the periwound edges dry.
- Apply protective skin barrier (Coloplast® Prep) to the periwound edges.
- Let dry and then re-apply.
Peristomal moisture-associated dermatitis
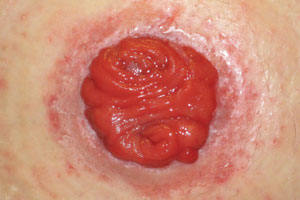
Caustic moisture damage: stoma effluent
Inflammation around a stoma due to sustained contact of stool or urine on the peristomal skin.
Interventions
- Assess cause of peristomal damage.
- Prevent any further damage (i.e., cut ostomy barrier to size, change pouch according to schedule, change pouch immediately for burning or irritation).
- Gently wash the peristomal skin before applying a new pouching system. Pat dry.
- If skin is moist and weepy, consider managing with crusting technique (Ostomy Powder and Coloplast® Prep).
Candidiasis
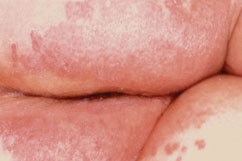
Yeast infection
A yeast infection of the skin caused by candida fungus. Commonly found in warm, moist areas, such as skin folds. Characteristics include small pustules and a macerated beefy red rash with satellite lesions.
Interventions
- Assess and treat cause.
- Gently wash with a pH-balanced skin cleanser. (Bedside-Care® Foam or EasiCleanse™ Bath Cloths)
- Management options:
- May use a topical antifungal (Micro-Guard® powder or Baza® Antifungal cream).
- When incontinence is present: apply antifungal moisture barrier (Critic-Aid® Clear AF)
- For skin folds: use InterDry® Ag to eliminate friction, moisture & bacterial/fungal bioburden.
Xerosis
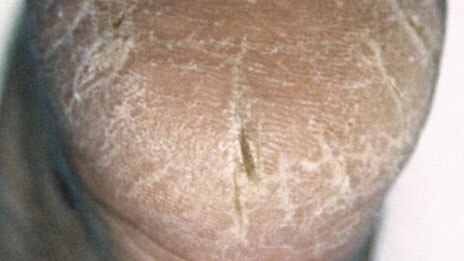
Dry skin:
An abnormal dryness of the skin. Characteristics include dry, scaly, itchy, red skin. May have fissures and cracks. Arms, legs and heels are commonly affected. Pruritus may be present.
Interventions
- Assess and treat cause of dry skin.
- Gently wash with a pH-balanced cleanser (Bedside-Care® Foam or EasiCleanse™ Bath Cloths).
- Apply moisturizer to skin at least daily and PRN (Sween® 24).
- To exfoliate extremely dry/fissured skin, such as heels use moisturizer with urea and lactic acid (Atrac-Tain® Cream).
Erythrasma
A bacterial infection caused by corynebacterium minutissimum. Characteristics include a reddish-brown, slightly scaly patch with sharp borders, occurring in moist areas such as the groin, axilla, and skin folds. Pruritus may be present.
Interventions
- Assess for cause of skin irritation.
- Gently wash with a pH-balanced cleanser. (Bedside-Care® Foam or EasiCleanse™ Bath Cloths)
- Management options:
- May treat with a topical antibacterial.
- For skin fold/under medical device: use InterDry® Ag to eliminate friction, moisture & bacterial/fungal bioburden.
Tinea Cruris
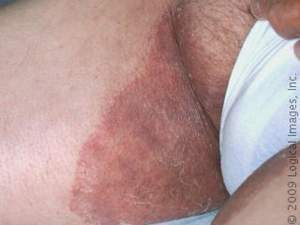
Jock itch
A fungal infection of the groin caused by friction and perspiration. Characteristics include an itchy, red, scaly rash that can spread from the groin to the genitals, inner thighs, buttocks and anus.
Interventions
1. Assess and treat cause.
2. Gently wash with a pH-balanced cleanser. (Bedside-Care® Foam or EasiCleanse™ Bath Cloths)
3. Management options:
• May use a topical antifungal (Micro-Guard® powder or Baza® Antifungal cream).
• When incontinence is present: use antifungal moisture barrier (Critic-Aid® Clear AF).
• For skin folds: use InterDry® Ag to eliminate friction, moisture & bacterial/fungal bioburden.
Tinea Pedis
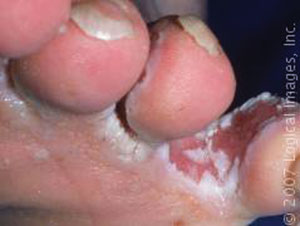
Athlete’s foot
A fungal infection in the foot. Characteristics include fissuring, maceration, scaling and burning between the toes.
Interventions
- Assess and treat cause.
- Gently wash with a pH-balanced skin cleanser (Bedside Care® Foam or EasiCleanse™ Bath Cloths).
- Management options:
- Use InterDry® Ag between toes to eliminate friction, moisture & bacterial/fungal bioburden.
- May use topical antifungals (Micro-Guard® powder or Baza® Antifungal Cream).
Pruritus ani
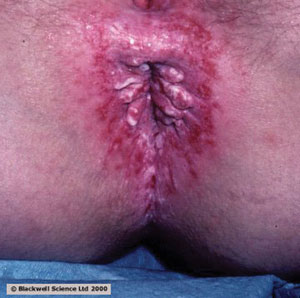
Chronic itching
An intensely itchy rash around the anus caused by exposure to irritants in the stool. Rash is worsened by vigorous use of toilet tissue or scrubbing with soap and water.
Interventions
- Assess for cause of skin irritation.
- Gently cleanse skin after each bowel movement with a pH-balanced, no-rinse perineal/skin cleanser (Bedside® Care foam, EasiCleanse™ Bath cloths or Baza Cleanse & Protect®).
- Apply skin protectant (Critic-Aid® Clear).